- Current status of ultrasonography in national cancer surveillance program for hepatocellular carcinoma in South Korea: a large-scale multicenter study
-
Sun Hong Yoo, Soon Sun Kim, Sang Gyune Kim, Jung Hyun Kwon, Han-Ah Lee, Yeon Seok Seo, Young Kul Jung, Hyung Joon Yim, Do Seon Song, Seong Hee Kang, Moon Young Kim, Young-Hwan Ahn, Jieun Han, Young Seok Kim, Young Chang, Soung Won Jeong, Jae Young Jang, Jeong-Ju Yoo
-
J Liver Cancer. 2023;23(1):189-201. Published online March 24, 2023
-
DOI: https://doi.org/10.17998/jlc.2023.03.11
-
-
1,605
Views
-
65
Downloads
-
2
Citations
-
 Abstract Abstract
 PDF PDF Supplementary Material Supplementary Material
- Background/Aim
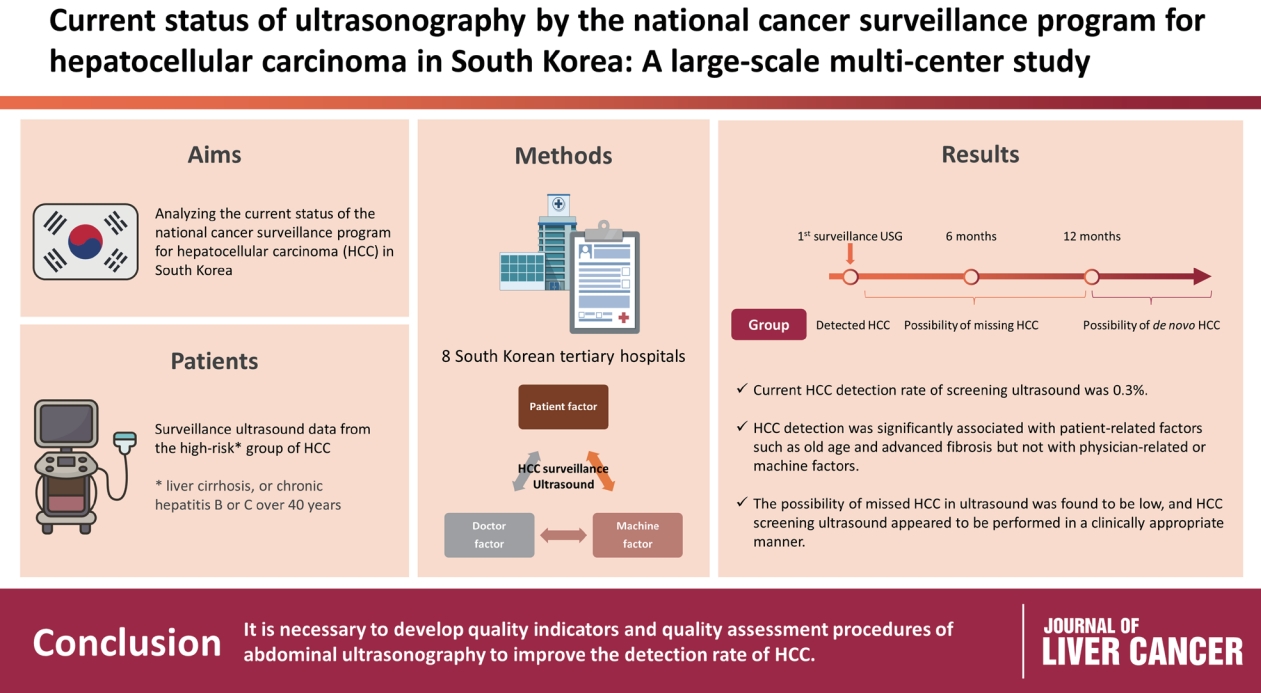
Abdominal ultrasonography (USG) is recommended as a surveillance test for high-risk groups for hepatocellular carcinoma (HCC). This study aimed to analyze the current status of the national cancer surveillance program for HCC in South Korea and investigate the effects of patient-, physician-, and machine-related factors on HCC detection sensitivity.
Methods
This multicenter retrospective cohort study collected surveillance USG data from the high-risk group for HCC (liver cirrhosis or chronic hepatitis B or C >40 years of age) at eight South Korean tertiary hospitals in 2017.
Results
In 2017, 45 experienced hepatologists or radiologists performed 8,512 USG examinations. The physicians had a mean 15.0±8.3 years of experience; more hepatologists (61.4%) than radiologists (38.6%) participated. Each USG scan took a mean 12.2±3.4 minutes. The HCC detection rate by surveillance USG was 0.3% (n=23). Over 27 months of follow-up, an additional 135 patients (0.7%) developed new HCC. The patients were classified into three groups based on timing of HCC diagnosis since the 1st surveillance USG, and no significant intergroup difference in HCC characteristics was noted. HCC detection was significantly associated with patient-related factors, such as old age and advanced fibrosis, but not with physician- or machine-related factors.
Conclusions
This is the first study of the current status of USG as a surveillance method for HCC at tertiary hospitals in South Korea. It is necessary to develop quality indicators and quality assessment procedures for USG to improve the detection rate of HCC.
-
Citations
Citations to this article as recorded by  - The Epidemiology of Hepatitis B Virus Infection in Korea: 15-Year Analysis
Log Young Kim, Jeong-Ju Yoo, Young Chang, Hoongil Jo, Young Youn Cho, Sangheun Lee, Dong Hyeon Lee, Jae Young Jang
Journal of Korean Medical Science.2024;[Epub] CrossRef - Long-Term HBsAg Titer Kinetics with Entecavir/Tenofovir: Implications for Predicting Functional Cure and Low Levels
Soon Kyu Lee, Soon Woo Nam, Jeong Won Jang, Jung Hyun Kwon
Diagnostics.2024; 14(5): 495. CrossRef
- An Analysis for Survival Predictors for Patients with Hepatocellular Carcinoma Who Failed to Sorafenib Treatment in Pre-regorafenib Era
-
Chan Uk Lee, Young-Sun Lee, Ji Hoon Kim, Minjin Lee, Sehwa Kim, Young Kul Jung, Yeon Seok Seo, Hyung Joon Yim, Jong Eun Yeon, Kwan Soo Byun
-
J Liver Cancer. 2019;19(2):117-127. Published online September 30, 2019
-
DOI: https://doi.org/10.17998/jlc.19.2.117
-
-
 Abstract Abstract
 PDF PDF
- Background/Aim
s: Sorafenib is the standard treatment for patients with advanced hepatocellular carcinoma (HCC). We aimed to investigate the prognosis predictors and the role of second-line cytotoxic systemic chemotherapy (CSC) in patients with advanced HCC after sorafenib discontinuation in the pre-regorafenib era.
Methods
From 2007 to 2015 in the pre-regorafenib era, the medical records of 166 HCC patients, who had permanently discontinued sorafenib, were retrospectively reviewed. For further analysis of survival factors after sorafenib treatment failure, we compared the survival of patients who had maintained liver function after second-line treatment with the best supportive care (BSC) group and selective BSC (SBSC) group.
Results
After discontinuation of sorafenib, median overall survival (OS) was 2.8 (1.9-3.7) months. The OS in patients who discontinued sorafenib due to adverse effect, progression, and poor clinical condition were 5.5 (2.4-8.6), 5.5 (2.2-8.9), and 0.9 (0.5-1.3) months, respectively (P<0.001). The independent predictive factors of survival after sorafenib failure were serum level of bilirubin and albumin, α-fetoprotein, discontinuation cause, and second-line CSC. In comparison with survival between second-line CSC and BSC group, the CSC group showed better survival outcome compared to the BSC group (10.6 vs. 1.6 months, P<0.001) and SBSC group (10.6 vs. 4.2 months, P=0.023).
Conclusions
The survival after sorafenib failure in patients who discontinued sorafenib due to progression and adverse effects was significantly better than in those who discontinued treatment due to clinical deterioration. In the pre-regorafenib era, patients who received second-line CSC showed better survival than those who received only supportive care after sorafenib failure.
- Factors Affecting Prognosis of Hepatocellular Carcinoma with Portal Vein Tumor Thrombosis: Implications for Future Therapeutic Strategies
-
Sang Jun Suh, Hyung Joon Yim, Dong Won Lee, Jong Jin Hyun, Young Kul Jung, Ji Hoon Kim, Yeon Seok Seo, Jong Eun Yeon, Kwan Soo Byun, Soon Ho Um
-
J Liver Cancer. 2017;17(1):60-71. Published online March 31, 2017
-
DOI: https://doi.org/10.17998/jlc.17.1.60
-
-
2,127
Views
-
23
Downloads
-
1
Citation
-
 Abstract Abstract
 PDF PDF
- Background/Aim
s: Hepatocellular carcinoma (HCC) with portal vein tumor thrombosis (PVTT)
exhibits poor prognosis. The aim of this study is to evaluate factors associated with survival of
HCC patients with PVTT to suggest better therapeutic options.
Methods
Patients with HCC which were newly diagnosed at three tertiary hospitals between
January 2004 and December 2012, were reviewed retrospectively. Among them, Barcelona
Clinic of Liver Cancer stage C patients with PVTT were identified. Factors affecting overall
survival (OS) were analyzed and efficacies of the treatment modalities were compared.
Results
Four hundred sixty five patients with HCC and PVTT were included. Liver function,
tumor burden, presence of extrahepatic tumor, alfa fetoprotein, and treatment modalities
were significant factors associated with OS. Treatment outcomes were different according
to the initial modalities. OS of the patients who received hepatic resection, radiofrequency
ablation (RFA), transarterial chemoembolization (TACE), hepatic arterial infusion chemotherapy
(HAIC), sorafenib, systemic cytotoxic chemotherapy, radiation therapy (without combination),
and supportive care were 27.8, 7.1, 6.7, 5.3, 2.5, 3.0, 1.8, and 0.9 months, respectively (P<0.001).
Curative-intent treatments such as hepatic resection or RFA were superior to noncurativeintent
treatments (P<0.001). TACE or HAIC was superior to sorafenib or systemic chemotherapy
(P<0.001). Combining radiotherapy to TACE or HAIC did not provide additional benefit on OS
(P=0.096).
Conclusions
Treatment modalities as well as baseline factors significantly influenced on
OS of HCC patients with PVTT. Whenever possible, curative intent treatments should be
preferentially considered. If unable, locoregional therapy would be a better choice than
systemic therapy in HCC patients with PVTT.
-
Citations
Citations to this article as recorded by  - Value of surgical resection compared to transarterial chemoembolization in the treatment of hepatocellular carcinoma with portal vein tumor thrombus: A meta-analysis of hazard ratios from five observational studies
Keera Kang, Sung Kyu Song, Chul-Woon Chung, Yongkeun Park
Annals of Hepato-Biliary-Pancreatic Surgery.2020; 24(3): 243. CrossRef
- A Case of Simultaneous Resection of Recurrent Combined Hepatocellular Cholangiocarcinoma and Hypovascular Hepatocellular Carcinoma
-
Tae Hyung Kim, Soon Ho Um, Sang Jung Park, Seung Woon Park, Han Ah Lee, Yeon Seok Seo, Young Dong Yu, Dong-Sik Kim, Joo Young Kim
-
J Liver Cancer. 2017;17(1):94-99. Published online March 31, 2017
-
DOI: https://doi.org/10.17998/jlc.17.1.94
-
-
 Abstract Abstract
 PDF PDF
- Liver cancer is more complex to treat compared to cancers in other organs, since liver function
should be considered. In addition, only a few patients can be applied curative treatment due to
advanced stage at diagnosis. Therefore, early stage detection is important and has been increased
through screening and surveillance programs using image modalities recently. However, it is still
difficult to diagnose small or hypovascular hepatocellular carcinoma (HCC) even using advanced
image modalties. In particular, hypovascular HCCs do not show arterial contrast enhancement
which is a typical finding of HCC on computed tomography (CT) and magnetic resonance
imaging (MRI). Those also account for a considerable portion of early HCC. We present 54 yearsold
man who had recurrent hypervascular and hypovascular nodules on three phase CT and
gadoxetic acid-enhanced MRI. The nodules were removed by surgical resection and confirmed
as combined hepatocellular-cholangiocarcinoma and well differentiated HCC respectively.
- A Case of Management for Hepatocellular Carcinoma with Lung Metastasis
-
Han Jo Jeon, Tae Hyung Kim, Soon Ho Um, Yeon Seok Seo, Hyun Seo Kim, Ki Joon Lim, Seung Woon Park, Han Ah Lee, Dong-Sik Kim
-
J Liver Cancer. 2016;16(2):129-133. Published online September 30, 2016
-
DOI: https://doi.org/10.17998/jlc.16.2.129
-
-
 Abstract Abstract
 PDF PDF
- Liver cancer is the 2nd most common cause of cancer related death in Korea. Especially,
patients who present extrahepatic spread of hepatocellular carcinoma (HCC) have a shorter life
expectancy (50% survival at 1 year and less than 4 months of median overall survival). Molecular
target agent like sorafenib was usually mentioned as a treatment for them, but that was still not
firmly established. We present a 75 year-old who had expanding nodular type of HCC. The mass
was removed by resection and radiofrequency ablation. However, lung metastasis were revealed
shortly after surgery. That lesions were treated with lenvatinib and systemic chemotherapy.
- Clinical Outcome of Completely Ablated Hepatocellular Carcinoma in Single Session in Patients with Decompensated Liver Cirrhosis
-
Min Seon Park, Soon Ho Um, Ho Sang Ryu, Yeon Seok Seo, Sun Young Yim, Chang Ho Jung, Tae Hyung Kim, Dae Hoe Gu
-
J Liver Cancer. 2014;14(2):139-142. Published online September 30, 2014
-
DOI: https://doi.org/10.17998/jlc.14.2.139
-
-
 Abstract Abstract
 PDF PDF
- Most cases of hepatocellular carcinoma (HCC) occur in the Asia-Pacific region and in patients
with underlying hepatitis B and C viral infection. Although surgical resection is the gold
standard for treatment of HCC, only a few patients are surgical candidates because of their
lack of hepatic reserve. Liver transplantation, which eradicates HCC and replaces damaged
noncancerous hepatic parenchyma, is regarded as the best treatment for HCC in patients
with decompensated liver cirrhosis. However, the shortage of donors limit its widespread
use. Furthermore, the long waiting time for liver transplantation allow for tumor progression
and reduce patient survival. Given this long wait, there is a reasonable clinical need in the
meantime for minimally invasive methods to avoid progression of HCC in patients with
decompensated liver cirrhosis. We herein offer our experiences of therapeutic efficacy and
complications of the procedure and the changes in liver function before and after TACE and
radiofrequency ablation in patients with HCC and decompensated liver cirrhosis, defined as a
Child-Pugh-Turcotte score above 7. (J Liver Cancer 2014;14:139-142)
- Two Cases of Small (< 1 cm) Hepatocellular Carcinoma
-
Jin Yong Jung, Sun Young Yim, Chang Ha Kim, Jin Dong Kim, Yeon Seok Seo, Hyung Joon Yim, Ho Sang Ryu, Min Ju Kim, Beom Jin Park, Soon Ho Um
-
Journal of the Korean Liver Cancer Study Group. 2012;12(1):37-41. Published online February 28, 2012
-
-
-
 Abstract Abstract
 PDF PDF
- Tumor size is one of the most important factors for decision of therapeutic plan and prognosis of hepatocellular carcinoma
(HCC). If the diagnosis of HCC is made earlier in its small size, the prognosis is better. However the diagnosis of small HCC
is not easy because small HCC lacks the typical clinical and radiologic feature. We experienced two cases of small HCC less than
1 cm that was confirmed after first treatment.
- A Case of Hepatocellular Carcinoma with Early Multiple Recurrences after Liver Resection
-
Jae Hong Ahn, Hyung Joon Yim, Seung Young Kim, Jeong Han Kim, Yeon Seok Seo, Seung Hwa Lee, Hwan Hoon Chung, Tae Jin Song, Hong Sik Lee, Sang Woo Lee, Soon Ho Um, Jai Hyun Choi, Ho Sang Ryu
-
Journal of the Korean Liver Cancer Study Group. 2009;9(1):29-32. Published online June 30, 2009
-
-
-
 Abstract Abstract
 PDF PDF
- Hepatic resection is a standard curative therapy for hepatocellular carcinoma (HCC) although only 10~30% of patients are
indicated due to advanced stage or poor hepatic reserve. Five year survival rate after resection was reported as a mean of
55% (25~93%), but cases of early recurrence after hepatic resection had poor prognosis. As early recurrence after hepatic
resection is the one of the most important factors that determines the prognosis, many investigators have been trying to
determine the factors associated with early recurrence. We report a case of early multiple recurrence of HCC after curative
hepatic resection probably due to microvascular invasion of tumor and too close resection margin. We would like to suggest
that additional prophylactic measures need to be sought in this group of patients because these factors may influence on early
recurrence.
- A Case of Massive Hepatocellular Carcinoma Treated by Hepatic Resection, which did not Respond to Transarterial Chemoembolization
-
Jeong Han Kim, Hyung Joon Yim, Seung Young Kim, Jae Hong Ahn, Ji Hoon Kim, Yeon Seok Seo, Seung Hwa Lee, Hwan Hoon Chung, Tae Jin Song, Hong Sik Lee, Sang Woo Lee, Jai Hyun Choi
-
Journal of the Korean Liver Cancer Study Group. 2009;9(1):63-66. Published online June 30, 2009
-
-
-
 Abstract Abstract
 PDF PDF
- Surgical resection is the treatment of choice for hepatocellular carcinoma (HCC) in non-cirrhotic patients. The optimal
indication for resection is a single tumor in a suitable location for resection. However, limit of the tumor size is not clear.
We report a case of successful hepatic resection in patients with massive HCC sized more than 15 cm that did not respond
to transarterial chemoembolization (TACE). A 49-year-old male patient had received TACE two times for massive HCC.
However, the tumor size increased. Right hemihepatectomy was performed despite the extensive tumor size and underlying
liver cirrhosis. Ascites and wound infection were developed after resection, but the patient’s general condition got recovered
soon. Until 6 months after surgery, recurrence has not been detected. However, distant metastasis was noted at 7th month.
Although recurrence with distant metastasis was noted, we think aggressive surgical approach prolonged this patient’s
survival.
- A Case of Hepatocellular Carcinoma with Bile Duct Invasion
-
Yeon Seok Seo, Beom Jin Park, Yun Hwan Kim, Soon Ho Um
-
Journal of the Korean Liver Cancer Study Group. 2008;8(1):69-73. Published online June 30, 2008
-
-
-
 Abstract Abstract
 PDF PDF
- Cholestatic type hepatocellular carcinoma (HCC), in which obstructive jaundice is presented as the initial
presentation of HCC, is rare. The prognosis of cholestatic type HCC is generally poor and most of the patients
die from cholangitis or sepsis. Although some authors reported cases of successfully treated cholestatic type HCC
with surgical resection, most of the patients are inoperable at the time of diagnosis. Several reports suggested that
transarterial chemoembolization (TACE) showed a beneficial effect in improving the survival time and therefore,
TACE should be tried as a first choice of therapy in patients with cholestatic HCC with sufficient liver reserve
function. We experienced a case of obstructive jaundice as the initial presentation of HCC. His obstructive
jaundice showed significant improvement after several sessions of TACE.
- A Case of Hepatocellular Carcinoma with Combined Treatment
-
Eun Sun Kim, Yeon Seok Seo, Hyun Chul Kim, Yun Hwan Kim, Soon Ho Um
-
Journal of the Korean Liver Cancer Study Group. 2008;8(1):111-114. Published online June 30, 2008
-
-
-
 Abstract Abstract
 PDF PDF
- Hepatocellular carcinoma (HCC) is an aggressive tumor that frequently occurs in the setting of chronic liver
disease and cirrhosis. It is typically diagnosed late in the course of chronic liver disease, with the median survival
following diagnosis of approximately 6 to 20 months. Although the mainstay of therapy is surgical resection,
several other treatment modalities may also have a role. The patient’s hepatic reserve often dictates therapeutic
options. Treatment options are divided into surgical therapies (i.e., resection, cryoablation, and orthotopic
liver transplantation), and nonsurgical therapies (i.e., percutaneous ethanol injection, radiofrequency ablation,
transarterial chemoembolization, systemic chemotherapy, or radiotherapy). Here we report a case of successfully
treated HCC with combined therapy of surgical and nonsurgical modalities.
- Metastatic HCC Developed in the Peritoneal Cavity after Hepatic Resection - A Case Diagnosed by PET
-
Yeon Seok Seo, Hyung Joon Yim, Jung Woo Choi, Yang Seok Chae, Won Hyeok Choi, So Young Kwin, Chang Hong Lee
-
Journal of the Korean Liver Cancer Study Group. 2006;6(1):77-82. Published online June 30, 2006
-
-
-
 Abstract Abstract
 PDF PDF
- Positron emission tomography (PET) can detect tumor by estimation of glucose metabolism of tumor cells. We
experienced the case of intraperitoneal metastatic hepatocelluar carcinoma (HCC) diagnosed by PET. 36 year-old
male patient had undergone hepatic resection for HCC. In the course of postoperative follow up, AFP level had
risen gradually. We checked the abdominal sonography, CT, and celiac angiography, but results were unrevealing.
To investigate hidden metastatic tumor, PET was performed and small tumor on the side of spleen was detected.
The tumor was removed by laparoscopic operation, and revealed as HCC. AFP level gradually returned to normal.
|